Demystifying Maximum Allowable Cost (MAC) in Pharmacy Benefit Management
Welcome to The Coy Pharmer, where we focus on cultivating clarity in the intricate world of pharmacy benefits. Today we are unpacking Maximum Allowable Cost, commonly referred to as MAC. This pricing mechanism plays a central role in how generic drugs are reimbursed across pharmacy networks, yet it remains one of the most misunderstood elements of pharmacy benefit management. For anyone reviewing pharmacy claims, negotiating PBM contracts, or analyzing drug spending trends, a clear understanding of MAC is essential.
DRUG PRICING INDEXES
3/16/20265 min read

In this Episode:
The Basics
Breaking Down the Acronym
Why MAC Exists
In Practice
Why MAC Helps Payers
Challenges for Pharmacies
PBM Balancing Act
The Fine Print
MAC List Sprawl
Take-Homes for Employers
Take-Homes for Resellers
The Basics of Maximum Allowable Cost
Maximum Allowable Cost is a reimbursement ceiling established by pharmacy benefit managers for multi-source generic drugs. Instead of reimbursing pharmacies strictly according to a percentage of a published list price benchmark, the PBM sets a maximum dollar amount it will reimburse for a specific drug.
This ceiling applies regardless of the manufacturer that supplied the product. Pharmacies may purchase the drug from different wholesalers or manufacturers, but the reimbursement cannot exceed the MAC price established by the PBM.
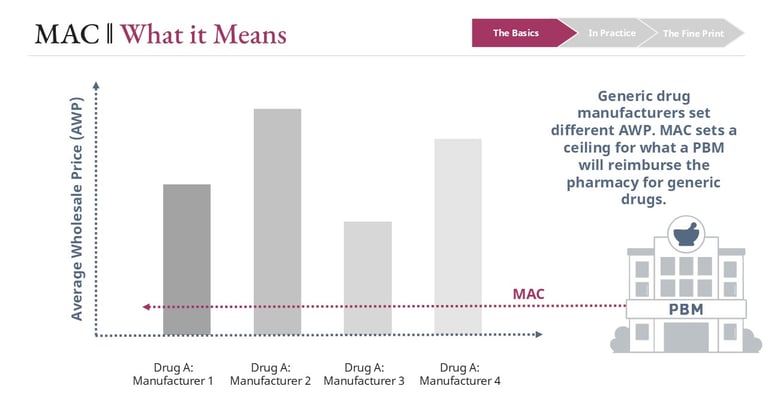
Why MAC Exists.
What Maximum Allowable Cost Means
The purpose of this approach is to ensure reimbursement reflects the competitive market price of generics rather than inflated list price benchmarks.
Generic drug markets behave very differently from brand drug markets. When multiple manufacturers produce the same molecule, prices often decline rapidly as competition increases.
If reimbursement relied entirely on benchmarks such as Average Wholesale Price, pharmacies could sometimes receive reimbursement far above the actual acquisition cost of the medication. In those situations, the reimbursement formula would fail to capture the savings created by generic competition.
Maximum Allowable Cost programs were introduced to address this problem. By establishing a reimbursement ceiling for widely available generics, PBMs can better align reimbursement with real market pricing.
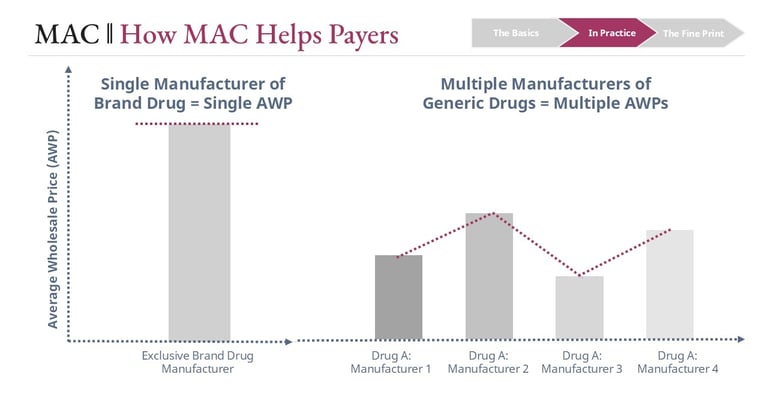
This approach helps plan sponsors capture savings when generics become inexpensive while still allowing pharmacies flexibility in how they source their inventory.
In Practice
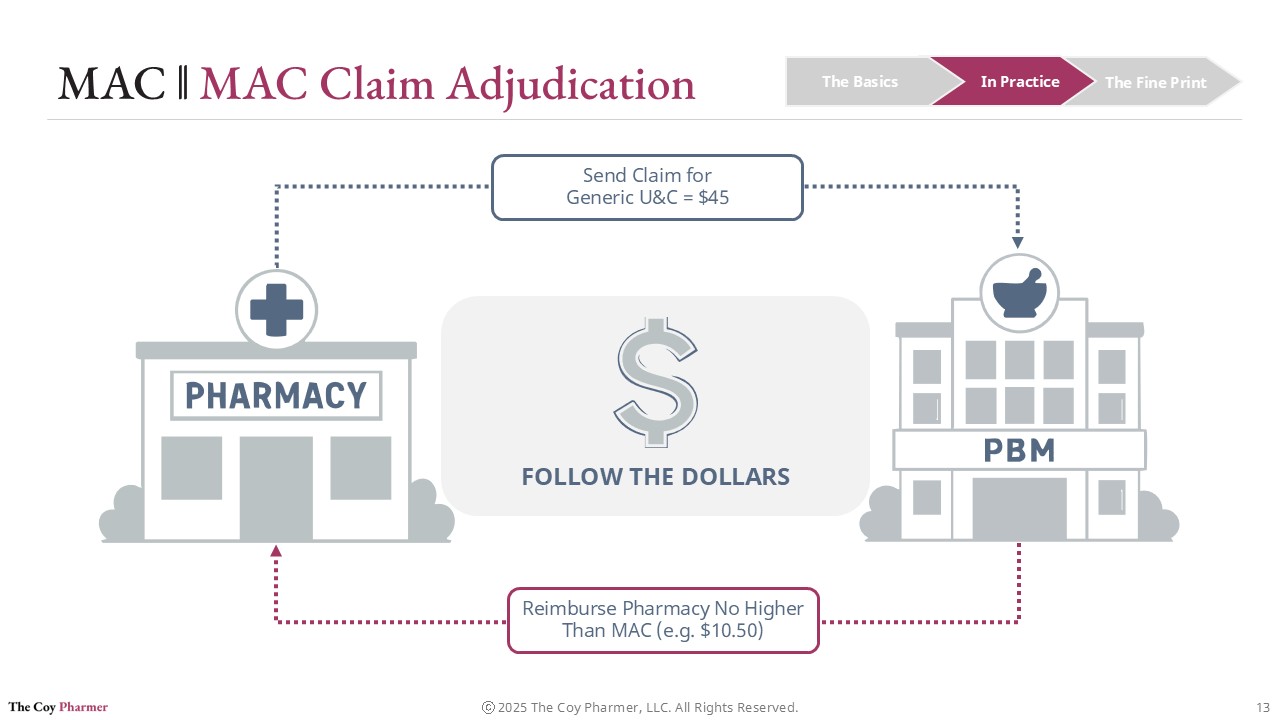
How MAC Works During Claim Adjudication
A typical pharmacy claim involves multiple pricing checks during adjudication. The PBM evaluates several potential reimbursement formulas before determining the final payment.
These formulas may include a contracted percentage discount off Average Wholesale Price, a usual and customary charge submitted by the pharmacy, and the MAC price if the drug appears on the PBM’s MAC list.
If the MAC price is lower than the reimbursement calculated using the contract formula, the MAC amount becomes the reimbursement ceiling.
Consider a simplified example.
The Average Wholesale Price (AWP) for a generic drug may be $100. A contract might reimburse the pharmacy at Average Wholesale Price minus 80 percent, which would result in a calculated reimbursement of $20. If the PBM’s MAC list sets the reimbursement ceiling at $12, the pharmacy will be paid $12 plus the dispensing fee (if applicable).
In this situation, the MAC price overrides the percentage of list price formula.
How MAC Lists Are Built
Developing MAC prices requires constant monitoring of generic drug markets. Pharmacy benefit managers use a variety of inputs to determine appropriate reimbursement ceilings.
These inputs may include purchasing data from pharmacies (such as National Average Drug Acquisition Cost – NADAC) , manufacturer competition levels, and market availability of the drug through major wholesalers.
Generic markets can shift quickly when supply disruptions occur or when new manufacturers enter the market. For that reason, MAC lists are typically updated frequently. Weekly updates are common, although some PBMs adjust certain prices even more often. Frequent updates are intended to ensure reimbursement remains aligned with the current market price of generics.
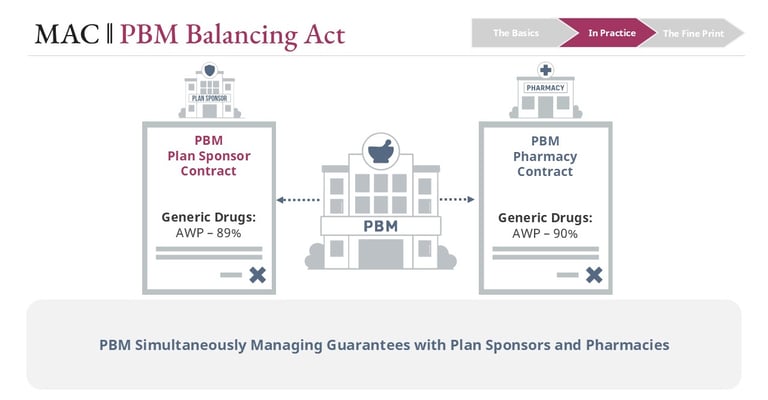
Pharmacy Benefits Managers often have guaranteed reimbursement floors set up with large chain pharmacies. This is often referred to as a “Generic Effective Rate” or GER. As PBMs work to balance contractual obligations to plan sponsors, they also must monitor performance of aggregate pharmacy reimbursement.
Performance relative to contractual guarantees can create financial pressure on both sides of the PBM model. When generic pricing performs better than the guarantees promised to the plan sponsor, additional value flows to the plan sponsor and PBM margin is reduced. When pricing falls short of those guarantees, the PBM may need to issue a reconciliation payment to the plan sponsor at year end, which can lead to dissatisfaction from the client.
A similar dynamic exists with large chains on the pharmacy side of the network. If reimbursement performs better than the guaranteed effective rate promised to pharmacies, additional value accrues to the pharmacy that the PBM cannot recover. If reimbursement falls short of that guarantee, the PBM may be required to issue reconciliation payments to pharmacies. These adjustments can generate complaints because they effectively reflect reduced cash flow throughout the prior year.
Maintaining equilibrium between plan sponsor guarantees and pharmacy reimbursement guarantees is a complex operational challenge. Even highly sophisticated PBMs must continually calibrate pricing mechanisms, including MAC lists, in order to manage this balance.
The Fine Print
MAC Appeals and Pharmacy Challenges
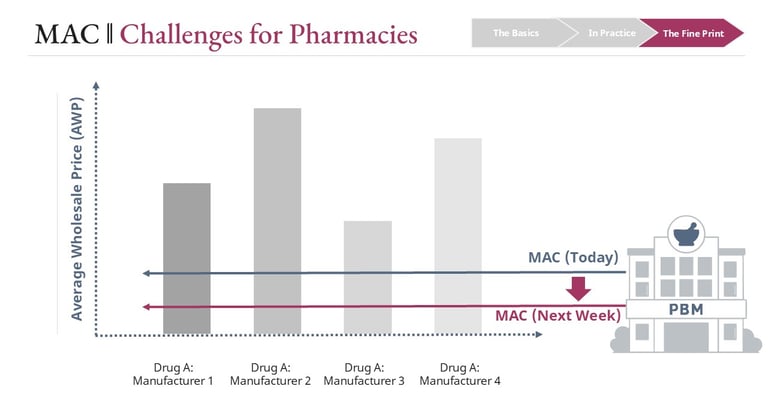
Despite the intention to reflect market prices, pharmacies often raise concerns that MAC reimbursement can lag behind real acquisition costs during supply disruptions.
When supply shortages occur, the acquisition cost of a generic drug may rise quickly. If MAC pricing does not adjust at the same pace, pharmacies may find themselves dispensing medications at a financial loss.
Many PBM contracts include a MAC appeal process that allows pharmacies to challenge reimbursement levels. Pharmacies typically must demonstrate that the drug cannot be purchased below the MAC level through standard wholesalers. Supporting documentation often includes wholesaler invoices and evidence that limited manufacturers are supplying the product. The effectiveness and speed of these appeal processes vary significantly between PBMs.
MAC List Sprawl
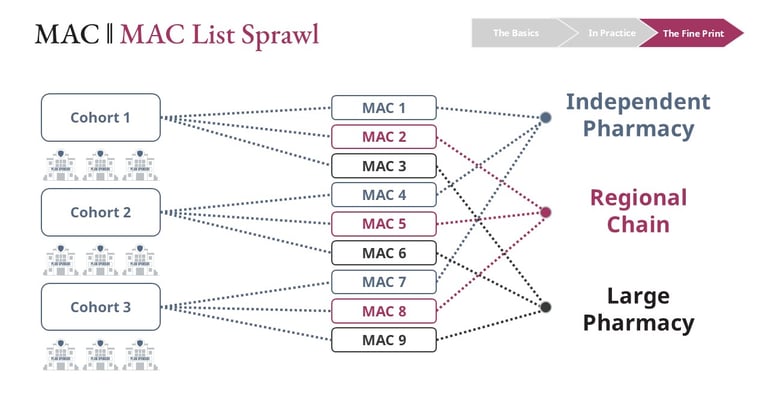
Another layer of complexity arises from the existence of multiple MAC lists within a single PBM.
Different pharmacy networks, employer contracts, and government program rules often require distinct pricing structures. Because of this, a pharmacy benefit manager may operate dozens or even hundreds of MAC lists at the same time.
This structure can produce situations where two members receive the same generic drug at the same pharmacy and appear to have the same benefit design, yet the underlying reimbursement is different. The difference occurs because their employers are associated with separate MAC lists, which can result in different generic reimbursement levels for the exact same medication.
At The Coy Pharmer, the goal is always to cultivate clarity in complex pharmacy benefit systems. Understanding how reimbursement benchmarks function is a foundational step toward evaluating PBM contracts and managing pharmacy benefit costs effectively.
Links
hello@thecoypharmer.com
© 2025 The Coy Pharmer, LLC. All Rights Reserved.
